 It is also easily attaches to most smartphones making it convenient to always have with you. In 30 seconds, it records a medical-grade EKG, which can be relayed to a doctor for analysis and diagnosis. Smaller than a credit card, KardiaMobile allows you to capture single-lead EKGs anywhere, anytime. Most commonly, PEA is caused by one of the following: Hypovolemia, hypoxia, acidosis, pericardial tamponade, tension pneumothorax, large pulmonary emboli, large myocardial infarction, hypothermia and/or drug overdoses.ĭo you know that 90% of the stroke could have been prevented? Resuscitation of the patient should focus on determining the cause of, and reversing the cause of this arrhythmia. Patients in PEA will have a rhythm (it can be any rhythm, technically speaking) on the monitor, but will be pulseless. 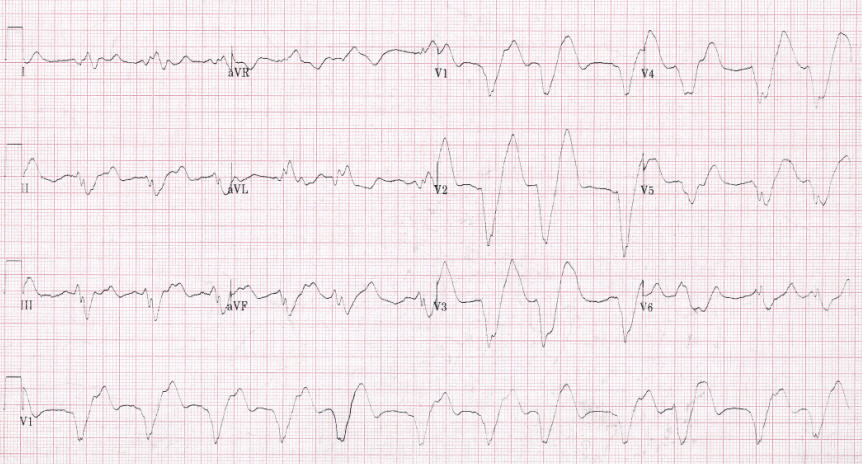
All rights reserved.Pulseless Electrical Activity (PEA), formerly known as Electromechanical Dissociation (EMD), is a condition in which there is electrical activity of the heart, but no mechanical capture (no mechanical pumping of the ventricles). No unique patterns were associated with the underlying causes or survival.Īetiology Cardiac arrest Causes Defibrillator Pulseless electrical activity Resuscitation.Ĭopyright © 2016 The Author(s). None of the patients with 'normal' PEA survived.Ībnormal ECG patterns were frequent at the early stage of in-hospital PEA. It occurs when the electrical activity in your heart is too weak to maintain a heartbeat or to pump blood through. Abnormal ECG patterns were seen in all survivors. Pulseless electrical activity (PEA) is a type of abnormal heart rhythm. Further 7 episodes with a corresponding defibrillator file, but without a reliable cause, were included in analysis of survival. No unique cause-specific ECG pattern could be identified. Ninety percent (46/51) had widened QRS complexes, 63% (32/51) were defined as 'wide-slow' due to QRS-widened bradycardia, and only 6% (3/51) episodes were categorized as normal. The defibrillator was attached after a median of one minute (75th percentile 3min) after the onset of arrest. 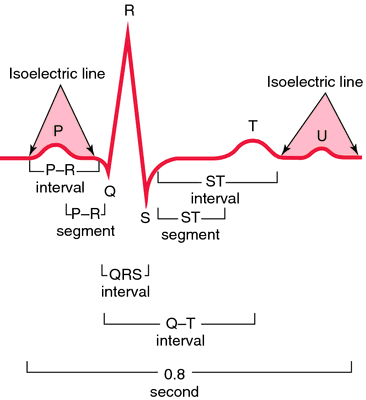
QRS width and HR were considered to be normal below 120ms and within 60-100 cardiac cycles per minute, respectively.įifty-one episodes fulfilled the inclusion criteria. QRS width, QT interval, Bazett's corrected QT interval, presence of P waves and heart rate (HR) was determined. Prospectively observed episodes of IHCA presenting as PEA between January 2009 and august 2013, with a reliable cause of arrest and corresponding defibrillator ECG recordings, were analysed. The aim of this study was to investigate possible associations between early ECG patterns in PEA and the underlying causes and survival of in-hospital cardiac arrest (IHCA). Pulseless electrical activity (PEA) is an increasingly common presentation in cardiac arrest. Olav University Hospital, Trondheim, Norway. 5 Department of Circulation and Medical Imaging, Norwegian University of Science and Technology, Trondheim, Norway Department of Anaesthesia and Intensive Care Medicine, St. 
4 Department of Circulation and Medical Imaging, Norwegian University of Science and Technology, Trondheim, Norway Department of Cardiology, St. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
